 Pathways to Medicaid Reimbursement for Pediatric Asthma Services
Pathways to Medicaid Reimbursement for Pediatric Asthma Services
EDITOR’S NOTE: This blog post is part of a national awareness campaign week focused on healthy communities. Follow online with #HealthyCommunities.
About 1 in 10 minors in the U.S. have asthma – that’s roughly 6 million children. Asthma is the third leading cause of hospitalizations for children under 15. At 13.8 million missed school days, it is a leading cause of school absences due to a chronic disease. Tragically, while most deaths caused by asthma can be prevented, this disease still claims the lives of 3,500 Americans each year. Children in inner-city areas are more likely to visit the emergency department or be hospitalized due to asthma attacks. Black children are six times more likely to die from asthma.
Asthma is a treatable and manageable disease, yet children are still regularly visiting the hospital with aggressive symptoms because they lack the resources and services to effectively reduce the triggers of severe attacks. To reduce the high rate of hospitalizations and ER visits, especially in low-income areas, communities have been exploring prevention measures such as in-school programs and home visits by nurses and community health workers. Community-based asthma programs also help families reduce asthma triggers by providing pest management services, hypoallergenic bedding, dehumidifiers, and special vacuum cleaners.
While these services are not traditionally considered billable health care, there are avenues available to states to offer coverage through Medicaid.
For example, New York and Oregon (see infographic) have used 1115 Medicaid waivers to provide preventative asthma services and supplies not otherwise covered by Medicaid.
In 2014, New York implemented the Delivery System Reform Incentive Payment (DSRIP) Program which promoted community-level collaborations. Among the eligible projects was home-based asthma management. (Watch the video.)
In 2012, Oregon used their waiver to develop Coordinated Care Organizations (CCOs) –networks of health care providers who have agreed to work together in their local communities to improve care delivery to Medicaid populations. These networks included community health workers and allowed reimbursement for non-traditional services to enhance asthma care.
One child who benefited from Oregon’s CCOs was Malik, who took part in a pilot program that focused on reducing home triggers while also providing nebulizers and inhalers. In the early 2000s, Malik was visiting the emergency room once or twice a month because of severe asthma attacks. By 2015, Malik was eight years old and had only visited the hospital twice due to asthma since entering CCO the pilot program. (Read Malik’s story.)
Treating, managing and reducing the burden of childhood asthma requires coordinated interventions that integrate community‐based approaches into patient care and take the management of asthma beyond the doctor’s office.
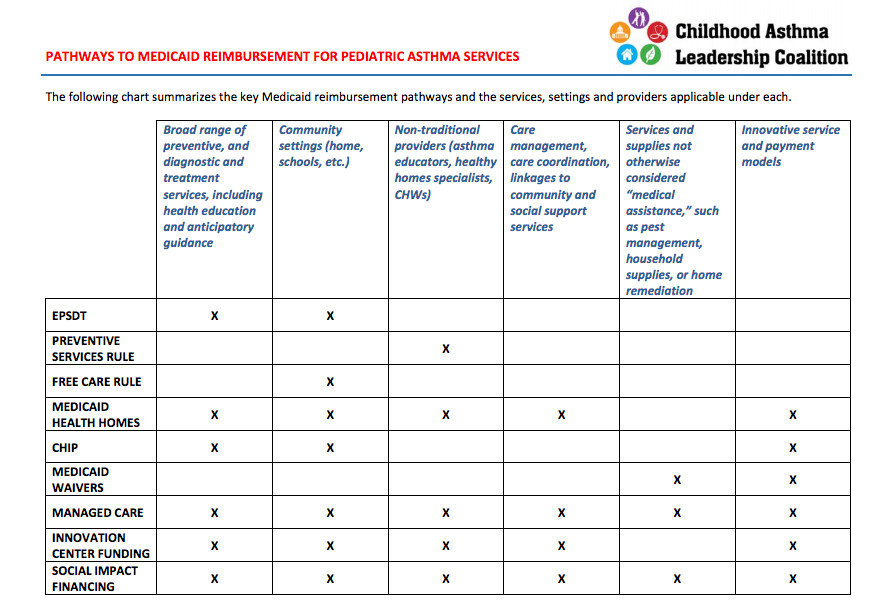
Evidence‐based, community‐focused interventions, which help children and their families to proactively manage their condition and mitigate asthma triggers, are fundamental to successful asthma control and show a significant return on investment. Medicaid offers several strategies for expanding these community‐based asthma programs. (See chart below.)
These preventative and innovative services empower families to manage asthma symptoms at home and in their community –keeping kids out of the ER and building #HealthyCommunities for all.
- Explore Childhood Asthma Leadership Coalition’s resources.
- Read Pathways to Medicaid Reimbursement For Pediatric Services Factsheet.
- Share your story. Use #HealthyCommunities to celebrate your community’s asthma programs.
- Join The Children’s Network to receive updates federal policies affecting kids’ health.