“There can be no keener revelation of a society’s soul than the way in which it treats its children.” — Nelson Mandela, May 8, 1995
Almost 25 years ago to the day, Nelson Mandela spoke these words. The health of our nation’s children is one of those tests.

In the coming days, Joe Biden and Bernie Sanders are working to establish joint policy task forces on the economy, education, criminal justice, immigration, climate change, and health care. These are all issues that are critically important to children and child advocates should be paying close attention. We will be urging those involved to carefully think about and consider how their policy proposals will impact and treat children.
Unfortunately, when it comes to public policy, children have often been treated as an afterthought. This has been true in health care policy discussions in the past, and is exemplified by how the Congress and the Trump Administration allowed the Children’s Health Insurance Program (CHIP) to expire for four months in 2017 and 2018. Child advocates remain hopeful but are still uncertain if this will change in the future.
Fortunately, in an interview with Ali Velshi on MSNBC earlier this month, Sen. Bernie Sanders was asked what he thinks would be a good fallback or first step since Medicare For All is unlikely to occur. Sanders replied:
At least what we should do is lower the eligibility age of Medicare from 65 to 55 and cover all of the children in this country, and then we can figure out ways that we can expand and improve the ACA. Those are some of the things that Joe Biden can do. . . .
A year ago, Vox’s Matthew Yglesias argued that a first step toward covering all Americans would be to “create a universal insurance program for children.”
Yglesias explained:
A Medicare for Kids program could accomplish a couple of key things. For one, it would cover the 4 million children who still lack health insurance. But beyond that, by simply and clearly guaranteeing coverage for all kids, it would offer peace of mind to all families that their children would have coverage no matter what happens. Last, it would offer a small subsidy to middle-class parents who are currently spending money for their kids’ insurance (both directly through premiums and indirectly through employer-size contributions), which would could help offset the enormous costs of parenting.
Leaving aside exactly what path this should take for the moment, the idea of “covering all kids” is particularly timely and welcome right now.
After the passage of CHIP in 1997, the uninsured rate for children dropped by more than two-thirds over two decades (15 percent in 1997 to just 4.5 percent in 2016). Unfortunately, due to the imposition of a number of new bureaucratic and administrative barriers to health care coverage by the Trump administration and states, progress for kids has reversed and the uninsured rate has increased to 4.3 million children or 5.5 percent in 2018.
Even worse, more children are losing coverage daily. In an American Prospect article, Joel Dodge explains:
The number of uninsured children will undoubtedly rise precipitously during the coronavirus crisis. When parents lose or change jobs, their children’s health coverage is often lost or disrupted too. But already during the coronavirus economic shutdown, a stunning 52 percent of people under age 45 — that is, around the age when people are raising a family — have either lost a job, been put on leave, or had their hours reduced.
In fact, in an analysis by the Urban Institute, they estimate that 6.6 million children would lose employer-sponsored insurance if the unemployment rate hits 20 percent. The report expects 90 percent of those kids would find alternative coverage through Medicaid, the Children’s Health Insurance Program (CHIP), or the Affordable Care Act (ACA) marketplaces, but that an estimated 700,000 children would become uninsured.

Coverage for Children Matters
Numerous studies confirm that coverage for children matters.
Every child in America needs and deserves to have affordable, comprehensive, high-quality health insurance coverage. During the last major debate over health care reform, a July 2009 National Opinion Surveys poll found that American voters supported “ensuring that all children have health coverage” by an 87–11 percent margin.
Every child deserves health coverage for health conditions like cancer, diabetes, heart disease, asthma, spina bifida, cystic fibrosis, acute flaccid myelitis (AFM), or any disabling condition, including the need for care during public health crises such as Zika and COVID-19.
Every child needs to have access to developmental screenings, physical and speech therapy, immunizations, mental and behavioral health services, vision care, and all other health care services, such as physician, hospital, and prescription drug coverage.
Ever since Medicaid was created in 1965, the goal of advocates has been to build upon that foundational coverage for low-income children to achieve coverage for all kids, just as Medicare has for people over the age of 65.
We have made tremendous progress in this country on the issue of children’s health. Since the passage of CHIP and up until the Trump administration, the improvement in children’s health coverage had been a national bipartisan success story.
First, Medicaid’s role in that success has been critical. Medicaid has provided the foundation for children’s coverage when it was created 55 years ago.
New York Times reporters Kate Zernike, Abby Goodnough, and Pam Belluck explain:
Medicaid now provides medical care to four out of 10 American children. It covers the costs of nearly half of all births in the United States. It pays for the care for two-thirds of people in nursing homes. And it provides for 10 million children and adults with physical or mental disabilities. . .
The program is so woven into the nation’s fabric that in 2015, almost two thirds of Americans in a poll by the Kaiser Family Foundation said they were either covered by Medicaid or had a family member or friend who was. The program not only pays for 16 percent of all personal health care spending nationwide, but also accounts for 9 percent of federal domestic spending.
In 2018, the Medicaid and CHIP Payment and Access Commission (MACPAC) estimates 36 million children received coverage through Medicaid at some point.
Medicaid works for children.
In 1997, the Children’s Health Insurance Program (CHIP) was created to give states the flexibility to either expand coverage for children through Medicaid or to allow states to build a separate but related health program specific to children whose families have too much money to qualify for Medicaid but not enough to afford private health insurance.
Over the last 23 years, CHIP has played a critically important role in the children’s health coverage system. MACPAC estimates 9.6 million children received coverage through CHIP at some point in 2018.CHIP is a bipartisan national success story.
The Future of Child Health
The American people understand that investing in the health of our children is investing in America and its future. When our children develop and thrive, we are paving the way for our country’s next generation of workers and leaders. And when our kids aren’t healthy, they do not learn and we will fail to stay the world’s leader in innovation.
Most Americans oppose the notion that children should be sick, live in pain, or go without preventive care like vaccinations and annual check-ups just because their parents have lost their job or simply can’t afford health insurance.
Today, health care coverage for children is at a crossroads. There are a few different directions our nation can take, but reversing course is not an acceptable path. Unfortunately, the Trump Administration’s policies have directly contributed to the increase in uninsured children.
These policies include:
- Increased bureaucracy and non-health related changes to Medicaid enrollment for adults and parents, including work requirements;
- Failure to pass an extension of CHIP in 2017 for four months;
- The chilling effect of the Trump Administration’s public charge rule and rhetoric related to immigration, which has undoubtedly led to a disproportionate increase in the numbers of uninsured Hispanic children;
- Slashed outreach and consumer assistance efforts; and,
- Increased bureaucracy and red tape in a few states.
Rather than seeking to fix these problems and reverse this negative trend, the Trump Administration’s budget proposal for fiscal year 2021 would make things even worse, as it recommends cuts to Medicaid and the Children’s Health Insurance Program (CHIP) by $920 billion over 10 years. Trump’s budget supports a 2017 legislative proposal by Sens. Lindsey Graham, Bill Cassidy, Dean Heller, and Ron Johnson to (1) “repeal and replace” the Affordable Care Act (ACA); and, (2) cap and cut Medicaid by block-granting the program.
It is important to highlight the proposed Medicaid budget cuts would likely disproportionately harm children. Adding insult to injury, the Trump budget also proposes to cut a few billion dollars out of CHIP.
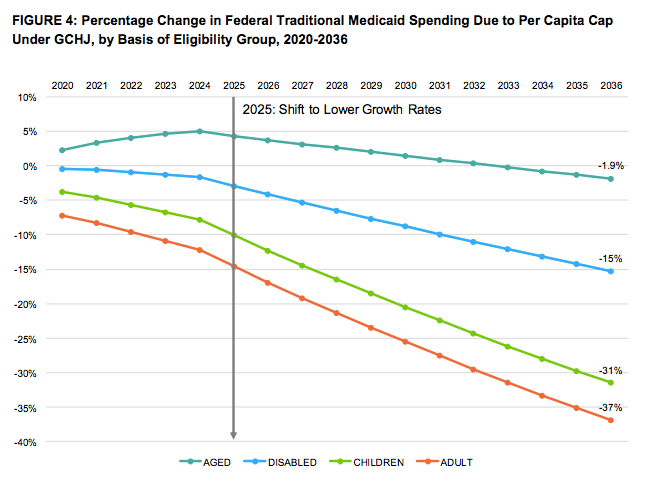
No child would benefit and millions would be harmed by such an approach. Fortunately, the Senate rejected it in 2017.

In contrast, others have crafted proposals that would seek to expand health coverage through some combination of a single-payer system or expansions of Medicare, the ACA, Medicaid, and/or CHIP.
In April 2019, Bryan Sperry, former president of the Children’s Hospitals of Texas, and I explained that there is a great deal of promise that some of these proposals “could achieve the goal of ensuring that all children have coverage. . . .”
But we also warned of “the potential harm, as some of these proposals completely repeal present coverage options for millions of children to be replaced with an entirely new system.”
Therefore, the question arises as to the best approach to cover all kids.
Children Have Unique Health Care Needs
First and foremost, any approach must recognize that children are not little adults. Children have unique health and developmental needs that are vastly different from adults, particularly senior citizens.
Children have special health care needs because they are immature and both their bodies and minds are developing and growing. Consequently, children are sometimes more susceptible to environmental toxins and certain diseases, but they are also typically more responsive to medical treatment and have a better ability to bounce back and heal from health challenges than others. This is why there is more of an emphasis on prevention, habilitation, and developmental milestones with children, as opposed to maintenance and rehabilitation for adults or senior citizens.
There is a reason we have pediatric medicine, pediatricians, pediatric nurses, and children’s hospitals. Children have special needs due to the fact that disease, stress and trauma, and health interventions are almost always different for kids than adults because they are growing and developing. Consequently, in a number of ways, pediatric care, supports, and services are quite different and can be more complicated than that for adults.
As an example, children often need habilitation, which aims to help a child develop motor skills that they have yet to accomplish. In contrast, rehabilitation, which is the focus of adult care services, refers to regaining skills, abilities, or knowledge that may have been lost or compromised as a result of illness, injury, or acquiring a disability.
In his book Healing Children, Dr. Kurt Newman, President and CEO of Children’s National, explains:
[Children] need specialty centers with doctors, nurses, psychologists, social workers, orderlies, administrators, and maintenance staff devoted to fostering an environment attuned to their unique psychology, biology, and medical conditions.
As a result, general hospital emergency departments sometimes fail to have the right-sized equipment to take care of children in all their developmental stages and sizes from infants, to toddlers, and up to adolescents. Among other things, children need different endotracheal tubs, resuscitation bags, laryngoscopes, suction catheters, intravenous catheters, needles, chest tubes, blood pressure cuffs, and medications. Children need more intensive and specialized pediatric nursing care, as children cannot be given instructions for self-care or left unattended in the same way adults are. Hospitals that care for kids must have expertise in child abuse and maltreatment. Children that have certain medical procedures, such as orthopedic and cardiology, sometimes have to repeat them as they grow and develop.
Even among children, there is an enormous array of different services and care needed. Babies are different from toddlers and their special needs, including services, equipment, and training required, are vastly different than those for adolescent medicine. As Dr. Newman says:
Babies are that different from children, as different biologically and anatomically as children are from adults. Medical intervention on infants, from surgical strategy to the calibration of anesthesia, from pain management to pain control, is completely different.
Unlike the rest of the health care system, CHIP recognizes these differences and has been developed to specifically address the needs of children. The benefits, the providers, the quality standards, the systems, the administration, etc. are all child-focused.
When you think about these differences, it becomes rather obvious. But somehow, when it comes to health care reform over the years, children are often not treated uniquely or with special consideration. Instead, they are often treated as an afterthought.
That must change. As Michael Freeman writes in his book The Moral Status of Children:
It is important that all those that formulate policy should be compelled to consider the impact their policies have on children.
Child advocates would urge that key principles should including:
- Making progress toward the goal of “covering all kids.”
- Recognizing that children need a pediatric health care system that is right-sized for their unique and special health care and developmental needs.
- Adopting a “do no harm” standard that asks and affirmatively answers this fundamental question: Is it good for the children?
“Medicare For Kids”?
For advocates pushing to get to universal coverage in this country, it is terrific that there are a number of voices pushing for children to be a first or top priority.
Like Yglesias, Dodge argues the American people would support an approach to expand coverage to all children and cites a recent Data for Progress poll in which, by a 60–32 percent margin, voters supported “extending universal health care to all American children by giving all Americans under the age of 26 coverage in a government health plan modeled off of Medicare, known as ‘Medicare for Kids.’”
However, “Medicare For Kids” means different things to different people. Some propose moving all children and young adults into the Medicare program, others would create a Medicare-like option on the Affordable Care Act (ACA) marketplaces in order to expand health coverage, and others would seek to create an entirely new Medicare-like system for children and young adults.
If children were all moved to Medicare, CHIP would be abolished (not sure what would happen to pregnant women covered by CHIP) and tens of millions of children would be taken out of Medicaid and moved into Medicare. Since Medicaid and CHIP were created with children in mind and have pediatric-specific benefits, pediatric networks, and stronger affordability protections than Medicare, this approach leaves child advocates with numerous questions as to how those protections and standards (built into Medicaid over the last 55 years and CHIP over the last 23 years) will be established and guaranteed in a new Medicare system. Employer health coverage of dependent children and individual market coverage would also be eliminated under this option.
Proponents of this approach point out that Medicare provides continuous enrollment without the need to repeatedly apply for coverage. The default is coverage and Medicare eligibility is based on age rather than income, although Medicare premiums and the prescription drug benefit are means-tested.
Opponents of moving millions of children into Medicare point out that, since Medicare is a program made for and dedicated to the care and treatment of senior citizens and people with disabilities, it lacks pediatric benefits, pediatric quality standards, pediatric provider networks, or much of anything with a focus on children. The only children receiving Medicare coverage are those with end-stage renal disease (ESRD). This is a significant concern and Medicare would need to be dramatically overhauled from top-to-bottom before children would be safely enrolled.
Medicare is also a far more complicated benefit than Medicaid or CHIP. Medicare has four different parts (Parts A, B, C, and D) and annual enrollment requirements related to Parts C and D.
Another concern is that Medicare’s premiums, deductibles, and out-of-pocket costs are much higher than Medicaid and CHIP.
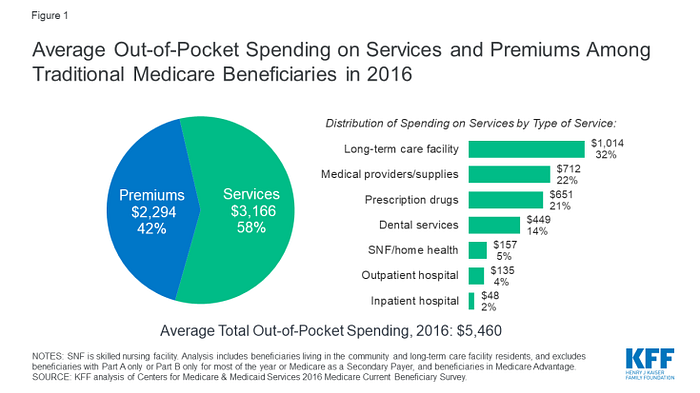
Medicare also lacks important benefits like habilitation, dental coverage, etc. that are critical to children. To compensate for this shortcoming, low-income senior citizens and people with disabilities (known as dual eligible) apply for Medicaid to provide a secondary or wrap-around cost-sharing and benefits while middle class and wealthier senior citizens and people with disabilities have secondary private insurance that acts as a wrap-around or they purchase Medigap coverage, which offers 10 different types of Medicare supplemental insurance.

The American people support the idea of “covering all kids.” However, by an overwhelming 3-to-1 margin, American voters have opposed eliminating or phasing out CHIP if it meant alternative coverage would be more costly for families and provide fewer benefits for children.
To ensure millions of children are not left worse off by this approach, Medicare would need to be kid-sized (radically change benefits, quality and access standards, and provider networks) AND radically changed to either:
- Eliminate most cost-sharing for all children;
- Means-test the coverage and benefit, much like Medicare prescription drug coverage, which makes Medicare more like Medicaid; or,
- Retain both Medicaid and CHIP to serve as secondary payers or wrap-around benefits for Medicare.
The first is politically impossible, the second undermines the major pro or point of moving coverage to Medicare, and the third is nonsensical.
In the latter case, it is critically important to highlight the role that Medicaid plays for children with special health care needs, including children with intellectual/developmental disabilities, physical disabilities, and/or mental health disabilities, and special populations like foster kids. Medicaid provides far more comprehensive services, including habilitative services and supports like transportation, targeted case management, and in-home care, including private duty nursing, attendant care, and assistive technology, that help children with special health care needs remain at home with their families, etc. than any other private health plan or Medicare does.
To address this shortcoming in other forms of insurance, Medicaid often becomes the secondary payer. In this context, it seems to make little sense to move millions of children out of Medicaid and CHIP but then have to retain Medicaid and CHIP to serve as secondary payers to cover those services and supports that Medicare fails to cover for children. Moreover, even that would not truly hold children harmless because having two forms of coverage with different requirements, standards, provider networks, etc. is far more complicated than one.
Finally, it is critically important to highlight that the health care system does not operate in a vacuum. Today state Medicaid and CHIP programs coordinate with WIC, Head Start, the Maternal Child Health (MCH) Block Grant, public health immunization projects, Ryan White HIV/AIDS, the Individuals with Disabilities Education Act (IDEA), the Indian Health Service (IHS), and the child welfare system. Efforts to improve developmental screenings, maternal depression, immunization rates, back-to-school campaigns, school health programs, and health services for foster kids are all critically important. These relationships happen at the state and local levels and something that is virtually impossible for Medicare to replicate.
Therefore, this all raises the obvious question as to whether Medicare, which is a program created for and focused on the health of senior citizens and people with disabilities, is the right program and approach for children, whether it could be dramatically overhauled to meet the unique and special needs of children, and whether it could be reoriented to ensure kids would not be less worse off or treated as a low-priority or afterthought.
Other “Medicare For Kids” pathways could entail modifying the ACA or creating a new health coverage program for children would face similar challenges and problems that moving children into Medicare would.
For example, we already know that ACA coverage for children has a lower actuarial value, fewer pediatric benefits, and yet, costs more than Medicaid and CHIP.
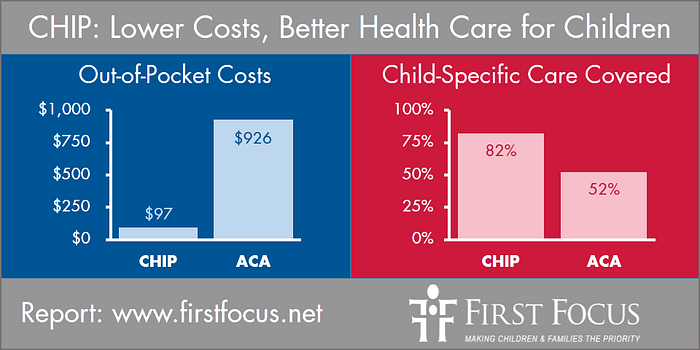
If the argument is to “simplify” coverage without leaving children worse off, an incredibly complex piece of legislation would need to be enacted that would radically overhaul pediatric coverage in either Medicare, the ACA exchange plans, or an entirely new program. This is anything but simple.

And that leads to the ultimate irony, which is that proponents of the elimination of Medicaid and CHIP are pushing for changes that would radically overhaul other forms of insurance to be more like . . . Medicaid and CHIP.
This begs the ultimate question: why end Medicaid and CHIP in order to try to recreate them?
Covering All Kids
Another approach or pathway favored by a number of child advocates would seek to adopt the best of all systems of care for children to get the country back on the road of progress.
This approach would build upon what is working for children in Medicaid, CHIP, the ACA, and private coverage while conforming to Sanders’s call to “cover all of the children in this country.” In fact, Sanders’s supporters should recognize that Sen. Sanders and Rep. Bobby Scott (D-VA) introduced legislation adopting such an approach in 2007, when 9 million children were uninsured, called the “All Healthy Children Act” (S. 1564).
As Rep. Scott said at the time, “How we take care of our children speaks to our very values as a society.”
A “Covering All Kids” approach would achieve the goal of providing coverage to the more than 4 million (and rising) uninsured children in this country today.
The following options are from ideas put forth by First Focus Campaign for Children in its “Proactive Kids Agenda,” the Children’s Hospital of Pennsylvania’s PolicyLab in its “Universal Health Coverage for Children: Current Barriers and New Paths Forward” report, and Georgetown Center for Children and Families in its “Covering All Children” options paper.
They include:
Eliminating Barriers to Care and Coverage: The first step would be to eliminate what does not work, which includes the increasing paperwork and bureaucratic barriers by the Trump Administration that prevent families from receiving health coverage and care for their children. Families should not be asked to fill out onerous and invasive forms, prove over and over that they are eligible for coverage, and jump through other bureaucratic hoops that are causing the number of uninsured children to rise in recent years.
Enrolling All Eligible Children: The majority of uninsured children in this country are eligible for but unenrolled in Medicaid or CHIP. Rather than move all children to Medicare, this approach would adopt a new expectation or default that all children and young adults below the age of 18, 21, or 26 would be covered.
This approach should include a combination of ways to enroll, retain, and renew coverage, including expanded outreach to families with children, such as enhanced use of culturally competent navigators, community health workers, and parent mentors; enrollment at key moments and places such as at birth and during enrollment in WIC, Head Start, early childhood, and education programs; simplifying paperwork and eliminating bureaucratic barriers; presumptive and express lane eligibility; continuous eligibility from birth under age six and at least 12 months or longer periods for younger children to eliminate churn and improve continuity of care; streamlined renewal of coverage; and, the elimination of any waiting periods in CHIP.
Information technology should be used to help families obtain and retain coverage for children rather than the reverse. The default should be coverage of children, just as it is for senior citizens in Medicare.
Making CHIP Permanent: CHIP works well for kids, but its major shortcoming is that it is temporary and includes out-year funding cliffs that make it vulnerable to political hostage-taking and gamesmanship when it repeatedly is set to expire. CHIP is the only federal health insurance program that is not permanent, which forces the child advocacy community to repeatedly have to push for extensions simply to maintain the status quo. Congress would never gamble with the coverage of senior citizens in Medicare or their own coverage, and nor should they do that to children.
Dodge is right to point out this problem. However, Dodge’s proposed “Medicare For Kids” solution, which would abolish CHIP and move kids into Medicare, would be extreme, difficult to pass, and potentially harmful to kids. It is the right problem but the wrong solution.
Instead, a far more simple and direct solution that builds on what already works for children would be to pass bipartisan legislation by Reps. Abby Finkenauer (D-IA) and Vern Buchanan (R-FL) called the CARING for Kids Act (H.R. 6151) to make CHIP permanent.
Finkenauer points out, “Too many kids’ futures are on the line if CHIP funding expires even temporarily. This bill will cut out uncertainty and help protect the health and well-being of our next generation.”
Buchanan adds, “Investing in affordable health care coverage for our nation’s children saves money in the long run — and it’s the right thing to do.” We agree. It is time to protect the health of millions of children and make CHIP permanent.
Expanding CHIP to 300 Percent of Poverty: For families with incomes above current Medicaid or CHIP limits but who still cannot afford or do not even have an offer of employer coverage, states should be given the flexibility to expand CHIP eligibility up to 300 percent of poverty with higher cost states allowed to cover children up to 350 percent of poverty.
Allowing Families and Businesses to Buy-In to CHIP or Medicaid: Parents want what is the best for their children. If families and businesses find that Medicaid and CHIP would provide better pediatric care that is more affordable for their children, they should be allowed to buy-in to either Medicaid or CHIP, as five states already do and others are exploring.

Under current law, Medicaid and CHIP are able to enact “premium assistance programs” to purchase employer-sponsored health coverage for children, but the reverse should also be allowed. If Medicaid or CHIP is more affordable and provides better care for children, employers and employees should be able to buy-in to that coverage. Parents and businesses should be allowed to do what is best for children.
Eliminating Medicaid Block Grants for Everybody: Medicaid is a critically important insurance program that is there for individuals and families when it is needed. That must be protected. The current dual COVID-19 and economic crises highlight two of the many reasons why it makes no sense to arbitrarily cut, cap, or limit Medicaid coverage through the imposition of block grants.
Health care needs and costs rise during economic recessions, natural disasters, public health epidemics, changes in demographics (i.e., a rapidly growing elderly population or population growth), advanced technologies that promote cures to health problems, etc. and Medicaid automatically adjusts for such changes. Unfortunately, the Trump Administration has repeatedly pushed for such caps and hundreds of billions of dollars in cuts to Medicaid coverage for millions of children, people with disabilities, adults, and senior citizens.
Medicaid block grants should be rejected, and that should include lifting arbitrary caps on funding for Puerto Rico and the territories that is devastating their health care systems and the care of children.
Covering Legal Immigrant Children and Pregnant Women Without Waiting Periods: Under the Personal Responsibility and Work Opportunity Reconciliation Act (PRWORA) of 1996, states are required to impose a five-year waiting period for children and pregnant women to receive coverage. Under the Children’s Health Insurance Program Reauthorization Act of 2009 (CHIPRA), states were given the option of waiving the five-year prohibition on coverage. As of January 2020, 33 states and the District of Columbia have waived the five-year waiting period for qualified, lawfully residing children and pregnant women in this country.
No child with cancer, asthma, spina bifida, cystic fibrosis, etc. or that needs eyeglasses, mental health services, or COVID-19 testing and treatment should be asked to wait five years to get necessary health coverage. Furthermore, it is ludicrous to ask pregnant women to wait five years to get health care. These barriers to care for children and pregnant women should be eliminated.
Enact the Health Equity and Accountability Act: Passage of this legislation would help improve the health, equity, and well-being of all families and children, including immigrants, across the nation.
Improving the ACA Coverage of Dependents: The ACA has successfully reduced the uninsured rate for millions of people across the country but has had less impact on the health coverage of children. One major barrier is that the ACA’s affordability provision or “family glitch” has had the inadvertent effect of making it more difficult to cover dependents, including children. A component of a “Covering All Kids” health reform should also address this unintended “glitch” for dependents.
The proposals cited in this section all meet the following principles:
- Making progress toward the goal of “covering all kids.”
- Recognizing that children need a pediatric health care system that is right-sized for their unique and special health care and developmental needs.
- Adopting a “do no harm” standard that asks and affirmatively answers this fundamental question: Is it good for the children?
These ideas all build upon and improve our health system to promote a healthy start in life, the growth and development of children, and improved equity.
In 2016, the uninsured rate for children had dropped to a record low 4.5 percent. Unfortunately, health coverage for children has declined under the Trump Administration.
Now is the time to embrace our past success, build on what works, fix what doesn’t, and get our nation back on the path toward “Covering All Kids.”
