The health of the child is the power of the nation.
— U.S. Children’s Bureau and Woman’s Committee on the Council of National Defense, 1918
 In 1997, a Republican-led Congress passed and President Bill Clinton signed into law landmark legislation, the Balanced Budget Act (BBA) of 1997 that included language creating the Children’s Health Insurance Program (CHIP). That legislation included provisions that a number of child advocates felt were a “triple-win” for children at the time.
In 1997, a Republican-led Congress passed and President Bill Clinton signed into law landmark legislation, the Balanced Budget Act (BBA) of 1997 that included language creating the Children’s Health Insurance Program (CHIP). That legislation included provisions that a number of child advocates felt were a “triple-win” for children at the time.
First and foremost, under the bipartisan leadership of Senators Edward Kennedy (D-MA), Orrin Hatch (R-UT), Jay Rockefeller (D-WV), John Chafee (R-RI), Bob Graham (D-FL), and William Roth (R-DE), BBA created CHIP in order to address the crisis in which 10.7 million children (15 percent) across the country were living without health insurance coverage.
As those who worked on the issue back in 1997 can attest, the lack of health insurance coverage among children was a national tragedy. In a report issued in 1991 by the bipartisan National Commission on Children entitledBeyond Rhetoric: A New American Agenda for Children and Families, Commission Chairman Jay Rockefeller wrote:
Perhaps no set of issues moved members of the National Commission on Children more than the wrenching consequences of poor health and limited access to medical care. In urban centers and rural counties, we saw young children with avoidable illnesses and injuries, pregnant women without access to prenatal care, families whose emotional and financial resources were exhausted from providing special care for children with chronic illnesses and disabilities, and burned-out health care providers asked to do more than is humanly possible.
If this nation is to succeed in protecting children’s health, there must be a major commitment from families, communities, health care providers, employers, and government to meet children’s basic health needs and to ensure that all pregnant women and children have access to health care.
 In fact, while one in seven of our nation’s children had no health insurance coverage, some places were far worse. For example, in El Paso, Texas, where I grew up, the Public Health Department reported that nearly 40 percent of the children were living without health coverage and many others were underinsured. Families were just an illness away from catastrophe and bankruptcy.
In fact, while one in seven of our nation’s children had no health insurance coverage, some places were far worse. For example, in El Paso, Texas, where I grew up, the Public Health Department reported that nearly 40 percent of the children were living without health coverage and many others were underinsured. Families were just an illness away from catastrophe and bankruptcy.
With that as the backdrop, there was bipartisan agreement that something had to be done. However, with a Republican-led Congress and a Democrat in the White House, compromise was necessary. Consequently, CHIP was a political bargain that created a federal-state partnership giving states,according to Eugene Lewit at the Stanford University Center for Health Policy and Primary Care and Outcomes Research, “considerable flexibility to innovate and tailor their programs to their specific circumstances, political climates, and timetables.”
Lewit adds:
. . .states succeeded in getting a large funding stream for many years and the flexibility to develop their own programs, including using Medicaid if they wished. Consumer groups got requirements on a comprehensive benefit package and limited cost sharing. Congress also included some accountability requirements, which also served to limit state prerogatives. The result was a win-win, as children’s coverage rates have grown almost every year since CHIP was enacted.
Another benefit of CHIP is that, by definition, it is a pediatric-focused system of care that recognizes children have special health care needs. Therefore, despite some initial challenges in getting all 50 states up and running and financing problems inherent in a quasi-block grant, CHIP has proven to be an enormous success story.
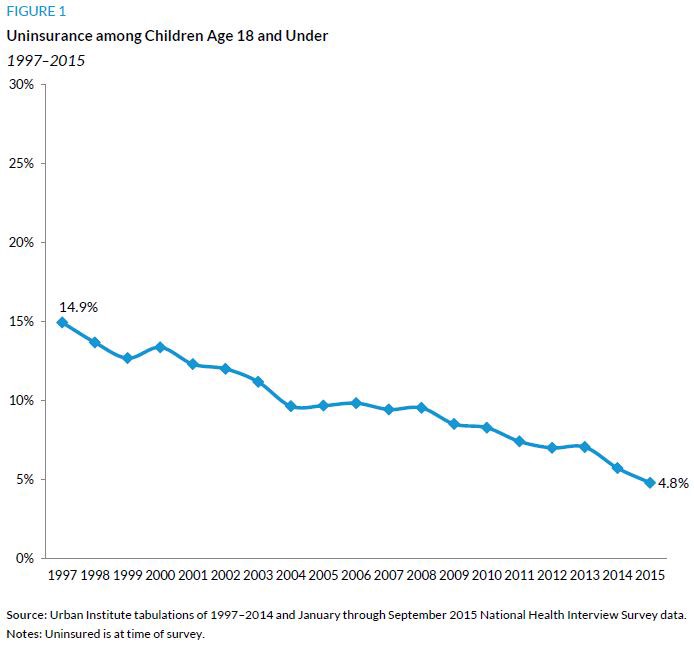
In fact, according to a report released this past week by the Urban Institute, “The uninsurance rate for children age 18 and under fell 67.9 percent between 1997 and the first three quarters of 2015, from 14.9 percent to 4.8 percent.”
CHIP has worked and that success is, in part, why the nation’s governors andover 1,500 organizations from across this nation successfully called for an extension of funding for CHIP last year.
Second, a tobacco tax was included in the 1997 law to help pay for CHIP.According to the Campaign for Tobacco-Free Kids, 36.5 percent of 12th graders were smoking in 1997 at the time the tobacco excise tax was imposed on cigarettes in the BBA to help pay for CHIP and reduce the federal deficit. Since then, the percentage of smoking 12th graders has declined to just 11.4 percent, which is a record low that represents a decline of 69 percent off the high in 1997.
And last, rather than failing to even pass a budget as Congress appears destined to do this year, Republicans and Democrats worked together in 1997 to enact the BBA, which the Congressional Budget Office (CBO) estimated would cut the federal budget by $127 billion over five years and helped lead to federal budget surpluses that materialized in 1998, 1999, 2000, and 2001. Both parties recognized that federal budget deficits were squeezing out the ability for Congress to respond to a range of national priorities, including investing in our nation’s children.
Thus, Congress passed CHIP, imposed a tobacco tax, and reduced the federal budget deficit — a “win-win-win” for children — that President Clinton signed into law on August 5, 1997.
Unfortunately, nearly 19 years later, the nation has allowed the federal budget deficit to grow again to the point where the Urban Institute estimates that, unless current budget policies are changed, “interest on the debt is projected to exceed spending on children from 2018 onward, by larger amounts every year.”
With respect to tobacco, there is a tax loophole that has developed with respect to roll-your-own tobacco and with the rapid growth in youth use of e-cigarettes, from 4.5 percent in 2013 to 13.4 percent in 2014, that should be addressed.
And with regard to CHIP, despite over 1,500 organizations from across the country expressing support for a four-year extension of the program last year, Congress acted to extend the program for just two years (or actually less since the extension included a financial “clawback” that raids out-year funding from unspent CHIP dollars that have historically rolled over and continued to be available to states to provide coverage to children). As professors Jonathan Oberlander and David K. Jones add:
The short 2-year extension of CHIP is itself a sign of problems. Democrats favored a 4-year extension but could not reach agreement with Republicans, partly because of a dispute over an ACA [Affordable Care Act] provision that provides states with enhanced federal CHIP payments. CHIP will go back up for a funding extension in 2017, and a new president and Congress will reconsider the program’s fate.
 Consequently, children’s and health care advocates are already getting organized for yet another battle to push Congress to protect CHIP, which currently provides health coverage to over 8 million children.
Consequently, children’s and health care advocates are already getting organized for yet another battle to push Congress to protect CHIP, which currently provides health coverage to over 8 million children.
Unfortunately for children, there are some voices that havesuggested children be moved out of CHIP and into the federal ACA Exchanges or to repeal CHIP and move it into Medicaid under a block grant or per capita cap. Under both of these scenarios, the health coverage of millions of children would suffer.
For example, according to estimates by the Urban Institute for the Medicaid and CHIP Payment and Access Commission (MACPAC), more than 1.1 million children could lose coverage altogether if CHIP were ended, due to limitations in the ACA Marketplace for children (i.e., both the family glitch and higher out-of-pocket costs).
And with respect to the imposition of a block grant or per capita cap upon Medicaid and CHIP, as proposed by the House Budget Committee, Edwin Park of the Center on Budget and Policy Priorities estimates that “[f]ederal Medicaid spending per beneficiary would be about 50 percent lower than under current law by the budget’s tenth year (2026).” Millions of children would potentially lose coverage if CHIP were eliminated and pushed into an arbitrarily capped or block granted Medicaid program.
As a nation, why would we take a U-turn and choose to wipe out all the gains and success we have made in children’s health coverage over nearly 19 years? We are so close to achieving the worthy goal of obtaining coverage and access to health coverage for every child in America. Now is simply not the time to backslide or undermine the success and gains for children that have been made over nearly two decades in Medicaid and CHIP.
Therefore, rather than putting health coverage for children at risk by eliminating CHIP and attempting to move them into ACA Exchange plans, underfunding both CHIP and Medicaid through the imposition of a state-by-state block grant or per capita cap, or disrupting private sector coverage with the “Cadillac tax”, we should strive to ensure all of our nation’s children are able to obtain high-quality and affordable health coverage.
In fact, with just 1 in 20 children in this country lacking health coverage, we are closing in on the goal of covering all children. In a recent study conducted by Dr. Glenn Flores and his colleagues that was published in Pediatrics, the authors looked into how to best reach and enroll the two-thirds of the uninsured children in this country who are eligible for but not enrolled in Medicaid or CHIP. The study found that “parent mentors” helped get children covered (particularly Hispanic and African-American children), improved health care access, and improved parental satisfaction. The biggest barrier to coverage was the lack of knowledge of parents that their children were eligible for either Medicaid or CHIP.
In the study, the use of parent mentors proved to be very effective at getting eligible but unenrolled children covered. As the Washington Post reported:
Ninety-five percent of kids whose parents worked with [parent] mentors were enrolled in insurance by the end of the study vs. 68 percent of controls, resulting in lower out-of-pocket costs, greater access to care and greater satisfaction among parents.
The agenda for children’s health coverage moving forward must be about getting to the finish line in terms of getting all children covered and improving their access to high-quality health care.
As Mark Wietecha, President and CEO of the Children’s Hospital Association wrote in The Hill:
Today’s generation of 80 million children represent the future leaders of our economy, our military, our public service, and are our entire future. We cannot afford to have their health status decline. . . . Let’s step up and take responsibility for ensuring our children have greater health and better lives, and are prepared to carry on the good and vitally important work of our country. It’s time to invest in our children, now.