EDITOR’S NOTE: This was originally published on Medium.
Now is the time for state leaders to stop being “wary” and to express their opposition to Trumpcare legislation moving through Congress with $772–834 billion in cuts to Medicaid between FY 2017–2026. The health of citizens across the country is at stake, and so is the fiscal health of states.
Both Moody’s and Fitch Ratings have sounded the alarm as to what this may mean at the state and local level. According to Fitch Ratings:
Fitch estimates the per-capita cap conversion makes up approximately $370 billion of the reduced Medicaid aid to states. . . Primary recipients of state funding, including local governments, public colleges and universities, and healthcare providers could be more pressured given their typically more constrained budgetary flexibility. Those entities more reliant on state aid, including Medicaid funding, would be particularly exposed.
On this point, we would also highlight a potential enormous negative impact to our nation’s public schools. Federal cuts to Medicaid could result in reduced funding to education if states divert state dollars to make up for the shortfall. Moreover, states could also cut Medicaid funding for certain services, such as special education in schools.
Trumpcare is not only a terrible deal — it is potentially the worst deal ever for states.
According to the Congressional Budget Office (CBO), Trumpcare would result in an unprecedented $772 billion in Medicaid cuts to states in the Senate bill and $834 billion in the House bill through FY 2026. The House and Senate bills also impose limitations on how the states choose to raise their own revenue, which will hamper the states’ ability to pay for the state share of Medicaid costs. And finally, the legislation dumps all of the responsibility for imposing the cuts that will be required by the bill upon the states.
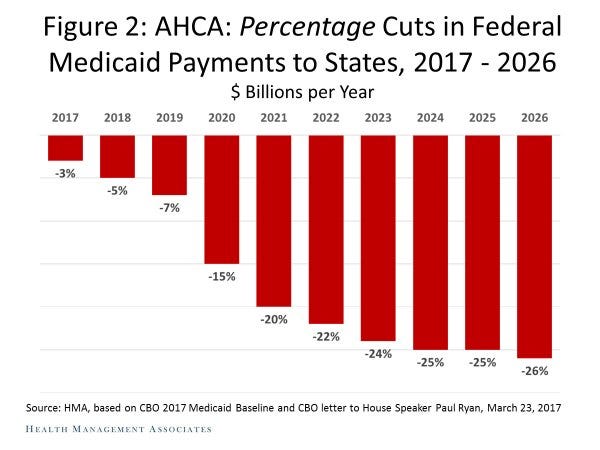
Based on these three major problems for states, some governors have spoken out against the bill. However, with cuts of this magnitude, you would think there would be far more governors and state legislators who would be telling their senators to oppose the legislation.
Fortunately, on Monday, the National Association of Medicaid Directors (NAMD) weighed in. As NAMD explains:
. . .no amount of administrative or regulatory flexibility can compensate for the federal spending reductions that would occur as a result of this bill. . . It would be a transfer of risk, responsibility, and cost to the states of historic proportions.
Maybe other state officials have remained silent because they will no longer be in office when the disaster strikes, even though that is irresponsible. Maybe some are so partisan that they only do what you are told by D.C. party leaders. But the fact is, state officials were elected to be leaders and have a responsibility to their states and citizens to stand up to what is a clear pending disaster.
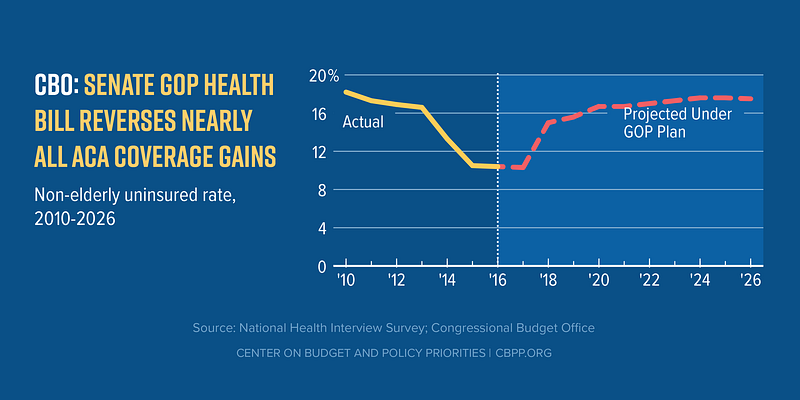
Governor John Kasich (R-OH) is one who has spoken out against the bill. On CNN’s “State of the Union” with Dana Bash on Sunday, Kasich said:
My job, as I see my job as a governor of a state — not as a Republican governor, but the governor of this state — my job is to look not just today, but in the out-years, at the impact it’s going to have on people who need help.
Kasich also said he recently saw 25 children eating at a Wendy’s, who were in Columbus, Ohio, for a Special Olympics event and thought:
‘Are these people being served? Are they going to be served by this bill in the future?’ My conclusion right now is no.
Standing up for what is right isn’t that hard, especially in light of what is at stake. As Kasich added:
. . .the fact is that you have to stand up on your own two feet, explain how you feel about things and be a leader. I don’t think we have enough leadership. I think there are too many people that cower in the wings because of partisanship. . . .
The Destruction of Medicaid
State leaders must speak out now, just as seven governors have done, on a bipartisan basis, in opposition to the legislation before Congress. These governors, which include Kasich (R-OH), John Hickenlooper (D-CO), Steve Bullock (D-MT), Charles Baker (R-MA), Brian Sandoval (R-NV), Tom Wolf (D-PA), and John Bel Edwards (D-LA), wrote a bipartisan letter to Senate Majority Leader Mitch McConnell in opposition to the House bill:
We believe that, first and foremost, Congress should focus on improving our nation’s private health insurance system. Improvements should be based on a set of guiding principles, included below, which include controlling costs and stabilizing the market, that will positively impact the coverage and care of millions of Americans, including many who are dealing with mental illness, chronic health problems, and drug addiction.
Unfortunately, H.R. 1628, as passed by the House, does not meet these challenges. It calls into question coverage for the vulnerable and fails to provide the necessary resources to ensure that no one is left out, while shifting significant costs to the states. Medicaid provisions including in this bill are particularly problematic. Instead, we recommend Congress address factors we can all agree need fixing.
After the Senate draft bill was released, they have confirmed their opposition to that bill as well.
Sadly, the Senate still hasn’t budged. Although the Senate has slowed the rate of the phase-down of the Medicaid expansion to adults that was included in the Affordable Care Act (ACA) in comparison to the House bill, the Senate’s Medicaid per capita caps are much worse.
In fact, the allowable inflation rate set in the draft Senate bill would start off with the House inflation rate caps and cuts in 2019 (set at CPI-M for children and adults and CPI-M + 1% for seniors and disabled), but then ramp down the allowable inflation rate dramatically. Beginning in 2025 and beyond, inflation would be arbitrarily set at much lower CPI-U, which is an inflation rate at around 50 percent below what Congress’s own Medicaid and CHIP Payment Advisory Commission (MACPAC) estimates is needed by states to retain current coverage for children, people with disabilities, and senior citizens. Cuts to states and the vulnerable populations Medicaid covers would be severe and compound over time.
CBO estimates that federal spending on non-disabled children and adults will grow faster, at 4.9 percent, than the allowable CPI-M, at 3.7 percent, but slightly slower than the allowable CPI-M + 1% for enrollees who are seniors or disabled under both the House and Senate bills.
However, in 2025 and beyond, CBO explains that the Senate bill’s shift to an inflation rate of just CPI-U would result in substantial Medicaid funding cuts. As CBO writes:
. . .the differences between spending growth for Medicaid under current law and the growth rate of the per capita caps for all groups would be substantial, as CBO projects the growth rate of the CPI-U in those years to be 2.4 percent.
A few senators have acknowledged that the lower inflation rate is unacceptably low but suggest opponents should “calm down” because there will be time to fix it before 2025.
However, nobody should count on that because the cuts would be so severe that Congress would have to find hundreds of billions of dollars in offsets to fix the problem this bill arbitrarily and wrongly creates today. Imposing such a burden on a future Congress and states is both irresponsible and potentially unfixable.
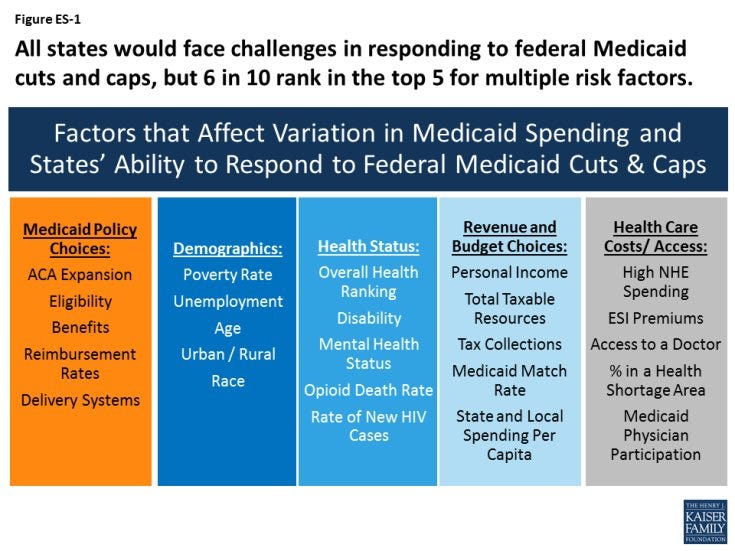
Furthermore, this one-sided, federally-imposed, and arbitrarily-set level of cuts and caps by Congress and President Trump in Medicaid pushes billions of dollars in cuts and harm down to the states with the falsehood and promise of “flexibility.”
The word “flexibility” is not magical. The cuts are so draconian that it will force states to use any newfound “flexibility” either to impose different levels of harm, such as raising taxes, cutting coverage, cutting benefits, cutting provider payments, or reducing access to care for millions of Americans.

The Hypocrisy and Unfairness of Federally-Imposes Medicaid Caps and Clawbacks
Furthermore, the Senate’s Medicaid per capita cap inflation rate that the federal government would pay states (2.4 percent) stands is far lower than the inflation rate that the federal government requires states to pay it (more than 11 percent over the last two years) for low-income prescription drugs as a result of the Medicare Prescription Drug, Improvement, and Modernization Act (Public Law 108–173).
Under that law, which was passed in 2003, Congress required that all low-income Medicare beneficiaries enroll in the new prescription drug program rather than through state Medicaid programs, as had historically been the case. Rather than allow states to save those dollars, Congress decided that they would require the states to pay for a large share of the costs for these low-income Medicare beneficiaries through the creation of a “clawback.”
The annual amount that states are required to pay the federal government is based on what states spent in 2003 on prescription drugs for low-income senior citizens and inflated by the U.S. Department of Health and Human Services (HHS) at an annual percentage index (API) in per capita drug expenditures in Medicare. Through this mechanism, states have been required to perpetually pay for a large and ever-increasing amount of the prescription drug costs of low-income Medicare beneficiaries, even though states no longer have any administrative or budgetary control over the program.
In sharp contrast to CPI-U, at 2.4 percent, that the Senate would be paying states for Medicaid, Congress imposed a far higher inflation rate on states for what it has to pay the federal government for Medicare prescription drugs. In fact, for the last two years, the API inflation rate imposed on states by the Secretary was 11.61 percent in October 2015 and 11.93 percent in October 2016 for the current year.
In short, Congress has created funding payment rates that inflate by double-digits when the states are paying the federal government, but a much, much smaller growth rate when the federal government is paying states. States get a horrible deal in both funding formulas.
Compounding the unfairness, the National Association of Attorneys General (NAAG) recently pointed out in a letter to Senate leadership that federal government fails to give states back its share of the Medicare prescription drug costs when it recoups billions of dollars in fraud and overpayments. According to NAAG:
Over the past decade the states have contributed approximately $80 billion dollars in monthly “clawback” payments to the Medicare Part D prescription drug benefit program. In 2017 alone, those clawback payments are expected to rise to over $11 billion. And over the past decade the Federal government has received, and continues to receive, millions of dollars in recoveries for fraud and overpayment cases involving Part D drugs. However, despite the states’ considerable — and growing — financial contributions to the Part D program, the states have not received a single dollar of those recoveries.
When Senator Ted Cruz was Solicitor General for the State of Texas, he was outraged by the unfairness of this breach of cooperative federalism. In a brief to the Supreme Court of the United States (SCOTUS) he, in fact, argued that the clawback should be declared unconstitutional.
In the brief to the Supreme Court, then-Solicitor General Cruz and others argued that the clawback “interferes with the States’ budgetary processes and eliminates the States’ control over a substantial portion of their budgets by tying their payments to the cost incurred by a federal agency over which the States have no control.”
The substantial portion of the clawback to state budgets was, according to the National Association of State Budget Officers, $9.35 billion for FY 2016.
If the $9.35 billion from the clawback is considered by states to be a “substantial portion” of state budgets, what about the federal impact of the Medicaid cuts in the Senate and House bills, which are estimated to be $772–834 billion between FY 2017–2026?
Furthermore, Cruz and others also contented that the prescription drug clawback “interferes with the States’ ability to govern” because the federal government “can arbitrarily raise or lower the States’ clawback payments when and how [it] likes.” The brief adds “there is nothing to prevent [the federal government] from similarly raising the amounts that the States owe in the future by manipulating the same variables used recently to lower the States’ clawback payments.”
Does this not sound quite familiar to the current debate in Congress?
First, between the House and Senate bills, the Senate bill arbitrarily manipulated and slashed the inflation rate downward for the federally-imposed per capita caps in FY 2025 and beyond. There is no policy rationale for that change — none whatsoever.
Second, while the Senate bill gives states the ability to request which quarters will count in their base for the purposes of calculating the 255 per capita caps that will be imposed upon states beginning in 2020, Section 133 of the Senate bill makes it clear that disputes over the quality of the data will be “determined by the Secretary” of the U.S. Department of Health and Human Services (HHS) and that “the Secretary may adjust the data as the Secretary deems appropriate.” States will have billions of dollars at stake and be put entirely at the mercy of HHS bureaucrats.
Third, the bill also makes it clear that the Secretary shall be solely vested with the authority to calculate the newly-imposed 255 Medicaid per capita caps and 51 total aggregate limits (the 50 states plus the District of Columbia). In that capacity, the Secretary might inappropriately calculate expenditures made in the State or the number of people enrolled in the past in the wrong category or the wrong quarter and that could throw off the calculation of the per capita caps in a number of categories or in the overall aggregate total limit.
Although the bill does allow a state to appeal the calculations, any appeal must be “filed by the State in such a form, manner, and time, and containing such information related to data errors that support such appeal, as the Secretary specifies.” Then and only then, the Secretary is solely vested with the decision-making to determine what is “valid.” Even if the Secretary finds that the appeal was correct and significant, any adjustments to fix the federal mistake “for a State may not result in an increase of the target total medical assistance expenditures exceeding 2 percent.”
Fourth, if the Secretary determines that a state has exceeded the “adjusted total medical expenditures” in a year, the Secretary will impose a new clawback upon states in the following year to recoup all the Medicaid spending that exceeded the cap in the previous year. There does not appear to be a provision in the bill that allows states to dispute the Secretary’s decision.
Finally, the Senate bill also requires the HHS Inspector General to undertake new auditing requirements to review each state’s spending “not less than once every 3 years.”
If $9 million strikes the states as unfair and potentially unconstitutional, states should be immensely more outraged by $772–834 billion in caps and cuts to the Medicaid program with all the terms of data collection, reporting, oversight, calculations, and disputes decided by the Secretary, who is unlikely to admit error and find in favor of the states if there is a dispute over how the caps should be enforced.
The one-sided and hypocritical nature of Medicaid caps and clawbacks should inspire every state official to contact their U.S. senators now.
Questioning the Constitutionality of Medicaid Per Capita Caps and Block Grants
In addition, Republicans in Congress have historically talked a great deal about states rights and most in Congress supported the Supreme Court decision’s in the National Federation of Independent Business v. Sebelius case to strike down the mandatory adult Medicaid expansion as unconstitutional state coercion. The Supreme Court decided that any expansion must be at the option of the states.
In that decision, Supreme Court Chief Justice John Roberts wrote:
In this case, the financial “inducement” Congress has chosen is much more than “relatively mild encouragement” — it is a gun to the head.
Under Roberts’s decision, states cannot be required to add a significantly new population because the alternative is to drop out of the Medicaid program entirely. However, under this rationale, wouldn’t an arbitrarily imposed per capita cap upon states, which shifts the risk of all future cost growth to the states with increased federal oversight of spending rules, also be unconstitutional? The federal government would be imposing these cuts upon states, which leaves states with no real choice other than to absorb the cuts. States would have no say in the matter.
As renowned Medicaid expert for recent chairwoman of the Medicaid and CHIP Payment Advisory Commission Sara Rosenbaum wrote in the New England Journal of Medicine:
For 50 years, the federal-state Medicaid compact has rested on the basic premise: in exchange for reliable, open-ended financing, states will entitle traditional populations to comprehensive benefits. Congress has altered the eligibility rules for traditional groups such as children, but as [Supreme Court Chief Justice John] Roberts noted, they were simply changes of degree, not kind. The federal compact stood untouched.
But the [per capita cap proposals before Congress] would cast aside the fundamental economic basis on which Medicaid rests and thus represent a dramatic shift in kind, not merely degree — fundamentally altering the program’s structure to achieve a purpose (shielding the federal government from health care costs) that was not part of the deal 50 years ago. The proposal would predicate ongoing federal funding on the states’ agreement to a new budgeting arrangement that forced them to access and absorb enormous financial risk by altering their obligations to pregnant women, children, and parents, while reducing long-term care commitments to elderly and disabled beneficiaries. By radically restructuring federal Medicaid financing, the [bills before Congress] becomes a legal “gun to the head”: a state that wished to receive continued federal Medicaid funding would be compelled to conform to a new compact. . . Legislation that would radically transform the federal-state Medicaid bargain without states’ consent may no longer pass the Tenth Amendment test.
Ironically, in other decisions by the Supreme Court, such as Armstrong v. Exceptional Child Center Inc., the federal government still has the authority to threaten Medicaid funding to states if the Secretary finds the state’s payments to providers are too low. Medicaid law also requires that states’ capitated payments to managed care organizations much be “actuarially sound”, which means they must be certified by a qualified actuary to cover reasonable, appropriate, and attainable costs in providing covered services.
As states face hundreds of billions of dollars in federal Medicaid cuts, they really only have a few options to cut: people, health care, or managed care and provider payments. States will be solely tasked with imposing the harm, while the federal government will retain the authority to demand that they not do so.
This will be a disaster for states and state elected officials unless they speak up now in opposition to this pending disaster.
Senate Bill Also Dictates States’ Taxing Authority by Limiting Provider Taxes
Furthermore, states have long protected their rights to collect and expand scare resources as they see fit. Unfortunately, Rosenbaum point out another enormous problem for states in the Senate bill. Rosenbaum explains:
At a time when states would lose hundreds of billions of dollars in federal funding and would be forced to find hundreds of billions of dollars in additional revenues to simply maintain their Medicaid programs, the Senate draft would impose new restrictions on states’ use of provider taxes. Broad-based and uniformly applied provider taxes have been an explicitly recognized feature of federal Medicaid policy since the early 1990s and are integral to the funding of state programs. . .
Current policy treats as permissible provider taxes that are no more than 6 percent of net patient revenues. The Senate draft would phase down lawful taxes to no more than 5 percent of net patient revenue by FY 2025, costing state Medicaid programs a major loss of revenue over the 10-year time period.
For a number of states, this will severely hamper their ability to raise the matching funding to pay for their share of Medicaid expenses — much less make up for the Medicaid shortfall caused by federal cuts.
States Will Be Required to Increase Bureaucracy and Red Tape
Some proponents of the Medicaid cuts argue states can simply cut out “waste.” However, the House and Senate bills, while cutting hundreds of billions of dollars out of state Medicaid programs, simultaneously require states to add to increased bureaucracy and red tape to comply with the bill’s new data collection, reporting, compliance, oversight, accounting, and audit requirements.
As I have pointed out, from a taxpayer’s point of view, the Senate bill is prioritizing the use of both federal and state dollars to have bureaucrats at both levels fight with each other every year over the data, accounting, and reporting on the numbers of people and spending levels in the five arbitrarily-imposed per capita limits that will be imposed upon every single state, rather than work together to ensure better health coverage to real Americans in need.
For example, for purposes of the per capita cap, is a foster kid with post-traumatic stress disorder and asthma defined as a child or disabled? Would a child count as enrolled before the end of a month or disenroll prior to the end of the month?
Or even more fundamentally, as Lisa Shapiro asks in a previous First Focus brief on the many problems inherent with per capita caps:
What constitutes enrollment for purposes of the per capita allotment? Is it at the time of application, eligibility approval, or assignment to a health plan? If a healthy child becomes disabled, do they move into that new category or is that risk assumed in the child subpopulation? How is the population of people with disabilities defined? Is a child with a mild form of hearing loss or severe asthma considered disabled and how do you define “mild” and “severe”?
Sadly, under a per capita cap regime, these questions will be a primary focus of both federal and state bureaucrats. What will be lost is any attention or focus on the actual quality and access to care for millions of Americans.
Nobody can rationally argue that the Senate bill will actually improve health care delivery to millions of Americans. It is, in fact, nonsensical and illogical to complain that Medicaid underpays providers but then propose cutting the program by hundreds of billions of dollars.
And yet, we can be assured that in a few years that the very same politicians that created this new and expanded bureaucracy at both the federal and state levels of government will decry “government-run health care” (even though they have it themselves and rush to defend Medicare and veterans’ health care coverage) as putting “government bureaucrats in the way of health care” and demand even further cuts to Medicaid.
In fact, they already are.
Finally, the Senate Bill Locks in Inequities Between States
In a blog entitled “Trumpcare’s Medicaid Cuts and Caps Create Losers and Bigger Losers,” I highlighted the enormous inequities in funding that will be permanently created by block grants and per capita caps. States should be concerned about the inequities and how the per enrollee amounts are calculated for all five categories of Medicaid enrollees should consult Figure 2 in Kaiser Family Foundation’s report entitled “Data Note: Variation in Per Enrollee Medicaid Spending.”
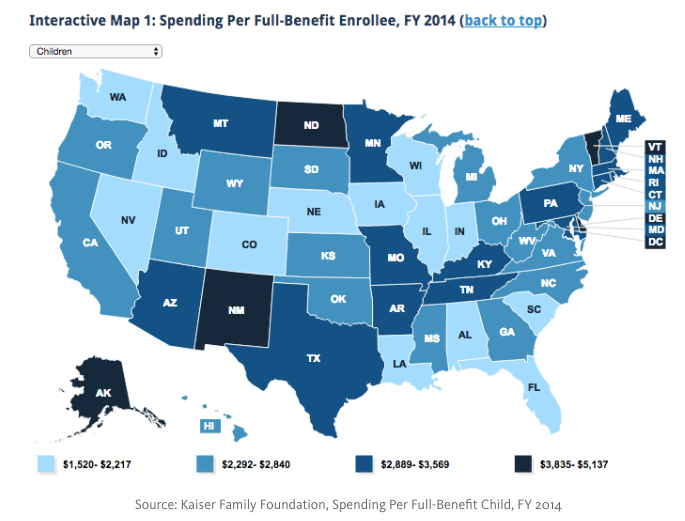
This is yet another issue about which state officials should undoubtedly be talking to their senators.
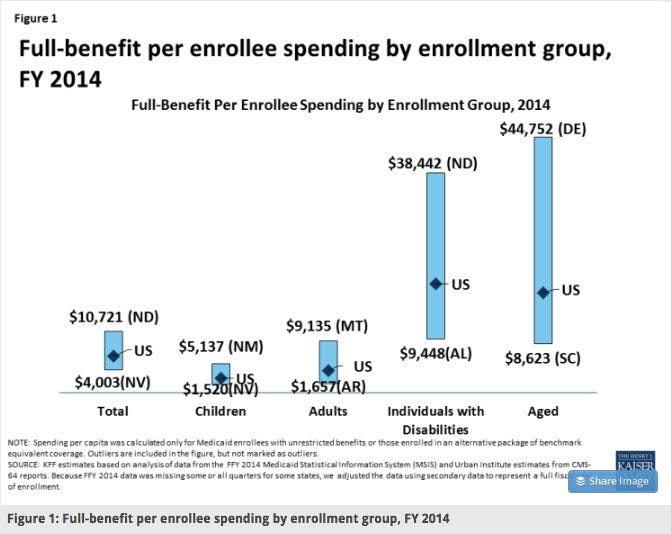
GOP Governors Bush and Beasley Were Right to Oppose Per Capita Caps in 1995
Finally, if state officials remain unconvinced, they should listen to Governors George W. Bush (R-TX) and David Beasley (R-SC). They argued strongly against Medicaid per capita caps at a Republican Governors’ Association press conference back on December 15, 1995. As they said:
Governor Bush: [Medicaid] per capita caps entitlements is a disaster, particularly when you are cutting the budget. And that’s what the President is asking us to accept and it’s a disaster.
Governor Beasley: Many of these Democratic governors are getting pressured from the White House. We understand that. It doesn’t change the fact that the President’s proposal on Medicaid will literally reap disaster on many states. South Carolina, for example, will have a substantial impact — a $3.3 billion impact on increased spending by South Carolina alone and that’s over a seven-year period, and that’s a state with a $4.1 billion budget.
To stop this pending disaster from taking effect, now is the time for state and local officials to call their senators at 202–224–3121 and demand that the federal government not impose per capita caps and block grants upon state Medicaid programs. This bill would be both a disaster for states and the millions of people that rely on Medicaid for their health care.
